By Marnie Werner, Vice President of Research
Ten years ago, I wrote a report on the opioid crisis in Minnesota and how it was masking an even bigger problem for Greater Minnesota, methamphetamine. In the following years, the addiction crisis rolled on, taking an unrelenting toll on lives and communities.
So imagine my surprise when I came across a new article in the Journal of the American Medical Association (“As US Overdose Deaths Drop, Researchers Search for Explanations”) talking about a drop in overdose deaths in the U.S.
It’s true, not just in the U.S. but in Minnesota, too, as the charts below show. Overdose deaths from the primary drugs fueling the epidemic have been declining over the last two to four years in all regions of the state except Southwest Minnesota. Why not there? More on that in a moment.
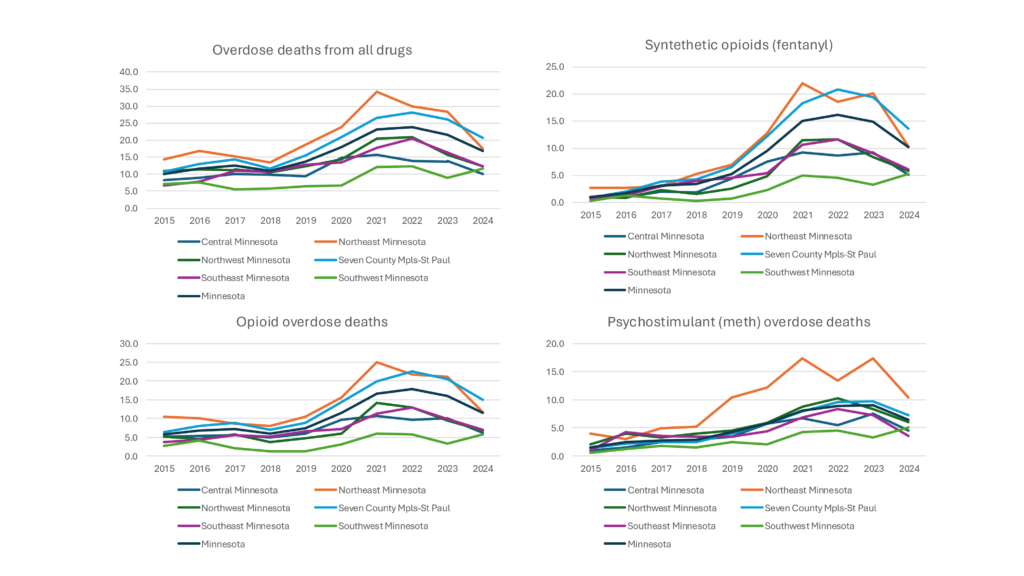
Figure 1: Between 2015 and 2024 (the latest data available), the rate of overdose deaths has dropped dramatically in most of the U.S., including in Minnesota. Meth, which accounts for about 98% of psychostimulant use, is not as big a killer as opioids and synthetic opioids (mostly fentanyl) but still plays a large role in the rural drug scene. (Note: Death rates shown here may differ slightly from other sources since we used 2024 population to calculate each year’s rate.) Data source: MN Department of Health.
Over the last 25 or more years, the United States has been dealing with a devastating epidemic of deaths driven by drug overdoses. The epidemic, says the JAMA article, in fact came in the form of three waves: the first one fueled by abuse of prescription opioids, the second wave by heroin overdoses, and the third wave by the introduction of synthetic opioids like fentanyl, hitting the East Coast around 2013, after which it “rolled through to the West Coast over the next few years.”[1]
But recent data now offers something that has been in short supply for a long time: cautious optimism. For the first time in years, overdose deaths are declining nationally, and importantly, that progress is reaching rural communities, too.
A Turning Point
Preliminary federal data shows that deaths from overdose declined in 2023 and dropped even more sharply in 2024, marking the most significant improvement since before the pandemic. Overdose is still a leading cause of death, for working-age adults especially, but this reversal gives hope.
The factors driving the decline are complex, the article states. It could just be an epidemic coming to its natural end, said Daniel Ciccarone, MD, MPH, a professor of addiction medicine at the University of California, San Francisco, in the JAMA article. All epidemics eventually burn out or become endemic, he said. Also, the population using illegal opioids is getting older, he added, and research suggests that the younger people coming behind them are using drugs less. There’s also a question of supply, especially around fentanyl. The article noted that in studying Reddit message boards where people discussed fentanyl, researchers found the word “drought” start to pop up in September of 2023, “then it rocketed up.”
So, access to supply could be a factor, too. When an illegal drug is scarce, dealers will mix less of it in with each dose, which, in the case of fentanyl, can make the drug less potent.
But restricting supply alone is not the reason and shouldn’t be expected to be a silver bullet, the article stated.
Why Rural Areas Are Seeing Improvement
Other factors have been at play, too, driving this shift. First, public awareness is growing. More people understand the risks of fentanyl and other synthetic opioids and now recognize the signs of overdose. Access to naloxone, the opioid overdose reversal medication also known by its brand name, Naloxone, has increased dramatically, even in smaller towns. Local public health agencies, community organizations, and first responders have worked to make sure the medication is available where it is needed most. Nearly 2 million prescription and over-the-counter doses were dispensed from retail settings in 2024, according to the article, and that didn’t count all the doses being made available through community-based organizations, emergency departments, hospitals, first responders, families, and people at risk themselves.
Second, treatment options have become more accessible. Telehealth has played an important role in rural areas, allowing residents to connect with providers without traveling long distances. More clinicians are also able to prescribe medications for opioid use disorder than in the past. On the policy side, the Substance Abuse and Mental Health Services Administration (SAMHSA) issued clear rules in 2024 on the use of medications for the treatment of opioid use disorder, including medications like buprenorphine and methadone, smoothing the way for their use.
Third, local efforts are paying off. An example is one we showcased in our report on access to mental health services for BIPOC communities in Greater Minnesota where residents of the White Earth Reservation launched their opioid addiction treatment program specifically for pregnant mothers. Basing it on not just modern medicine but also their own cultural practices and skills, they are helping mothers-to-be manage their addiction, allowing the mothers to deliver healthy babies and keep them.
These changes reflect a broader lesson: when resources are tailored to local needs and communities are engaged directly, rural areas can and do make meaningful progress.
What the Data Shows in Minnesota
Minnesota reflects these national trends. Preliminary data from the Minnesota Department of Health shows that overdose deaths declined by nearly a quarter between 2023 and 2024. Deaths involving opioids—and particularly synthetic opioids like fentanyl—fell even more sharply.
It may be that state and local efforts are gaining a foothold in the situation, too.
Most parts of Greater Minnesota saw meaningful declines right along with the Twin Cities metro area—a testament to the efforts going on across the state to address substance abuse and deaths from overdoses. It’s a meaningful shift: for instance, Northeast Minnesota, which has struggled for years with the highest rate of overdose deaths (rate of overdose deaths = number of deaths per 100,000 residents) has seen the largest improvement. From its peak of 34.3 deaths per 100,000 from all drugs in 2021, the rate has been cut in half to 17.4 in 2024.
For years, rural communities faced growing overdose rates alongside fewer resources for prevention, treatment, and emergency response, but the recent data suggests that targeted investments and local efforts are beginning to close that gap.
At the same time, the burden isn’t evenly distributed. Urban counties still account for a large share of total deaths, especially for opioid users, and some communities—particularly Native American populations—continue to experience disproportionately high overdose rates.
And in Southwest Minnesota, overdose death rates have stayed steady or even gone up since 2015. The reasons aren’t yet clear, but for one thing, Southwest Minnesota, like the rest of rural Minnesota, is dealing with a serious shortage of mental health care providers, including addiction specialists.
The JAMA article also offers another possible explanation. In talking about the fentanyl-fueled wave of deaths starting in the last decade, Ciccarone stated that the wave rolled from the East Coast to the West Coast over the next few years. “Following this regional pattern, eastern states such as Kentucky, Ohio, Pennsylvania, and West Virginia experienced earlier declines in overdose deaths, … while deaths in Alaska, Nevada, and Utah continued accelerating through October 2024.”
Maybe Southwest Minnesota just hasn’t hit its decline yet. In any case, there’s still work to be done.
What This Means for the Future
The recent decline in overdose deaths suggests that coordinated public health strategies combined with community-level action can save lives. For rural America, the data offers additional encouragement: progress is not limited to large cities, and in some cases, rural regions are leading the way.
But this is not the end of the story. Overdose deaths are still above where they were a decade ago. Disparities persist across geography and population groups. And the underlying drivers of substance use—economic stress, isolation, mental health challenges, and limited access to care—continue to affect communities everywhere, including rural communities.
Challenges to progress are still there, but this recent progress shows that change is possible. We can sustain and expand on what’s working: broad access to naloxone, effective treatment options, strong local partnerships, and culturally appropriate approaches for diverse communities. At the same time, we must remain vigilant as drug markets evolve and new risks emerge. The substance use problem can’t be solved overnight. But as the data is finally showing, recognizing, studying, and acting on those challenges is paying off in the form of lives saved.
[1] Anderer, Samantha. “As US Overdose Deaths Drop, Researchers Search for Explanations.” JAMA 335, no. 8 (2026): 656–57. https://doi.org/10.1001/jama.2026.0553.

